 I had finally found out the name for the slow, labor-like process I was going through all week. Our doula, my birth books and the nurses at my OB clinic referred to it as "prodromal" labor, which is a labor that takes place over the course of days, never picking up to full intensity long enough to go to the hospital, but never quite going away, even when contractions slow. Mine started on a Friday night, almost a week before Daniel was born. Prodromal labor in general is frustrating and emotionally taxing, and by Wednesday night, it had taken its toll on me. By then, the contractions had traveled from my lower back to my tailbone. They felt like horrible gas pains. Despite the intensity, they were only coming every 10 to 12 minutes, and from all I'd read, that wasn't close enough together to go to the hospital.
I had finally found out the name for the slow, labor-like process I was going through all week. Our doula, my birth books and the nurses at my OB clinic referred to it as "prodromal" labor, which is a labor that takes place over the course of days, never picking up to full intensity long enough to go to the hospital, but never quite going away, even when contractions slow. Mine started on a Friday night, almost a week before Daniel was born. Prodromal labor in general is frustrating and emotionally taxing, and by Wednesday night, it had taken its toll on me. By then, the contractions had traveled from my lower back to my tailbone. They felt like horrible gas pains. Despite the intensity, they were only coming every 10 to 12 minutes, and from all I'd read, that wasn't close enough together to go to the hospital. But on Thursday morning (Aug. 24), I did call my doctor's office. I wanted to ask about the leaking that had started early that morning. I couldn't tell if my water had broken or if my bladder was completely incontinent, caving into all the pressure on it. The nurse told me to go to the hospital and have it checked out. She sounded more urgent than I felt: If my water had broken, she insisted, the clock was ticking, and the baby had to come out within 18 hours or there was a risk of infection. (I questioned the 18 hour bit, but never mind.)
So Steve and I went over to United's birth center and checked into triage. Just to have this leaking checked out, I figured, and then we would go home. But lo and behold, not only had my water broken, I was also dilated to 6 centimeters! How on earth did I get that far and not know it? I tell you, I was so excited, I cried tears of happiness. This baby was about to be born! Or so I thought.
We called our doula ("six centimeters?!"), and she came over right away, wearing a cute blue sweat suit and a nametag identifying her as a member of Doulas of North America. Together, we were brought to the labor and delivery section and checked into room 2222. Alas, not enough staffing in the all-in-one rooms to let me have one. I was bummed, but it didn't matter in the end because the room we had was just fine. So was our first nurse, Lisa, who seemed tickled that we'd included a photo of ourselves in Ireland on our copy of our birth plan. We all chit-chatted for a while about Ireland, and that was a nice way to get to know each other.
All in all, we would go through three shifts of nurses, and except for the middle one, who wouldn't let me get back in the tub and wasn't as positive as I wished her to be, the nursing care we received throughout our stay was far better than I'd expected, given my initial misgivings about United. Our doula, who has attended births at many hospitals around the Twin Cities but never before at United, said she was blown away by how much respect and extra personal attention we received from everyone from the nurses to the anesthesiologist (even though he messed up my epidural) to the on-call doctors.
For first 12 hours of my labor at the hospital, we walked the halls of United, peeked into the nursery at the newborn babies, took a bath in the tub and later, when things got more intense, a shower. The hot spray felt so good against my lower back. When a contraction came, I stopped what I was doing and leaned against Steve, breathing through it. There was a storm that evening, and it felt refreshing and exhilarating to watch the lightening and wind and rain outside our window. And I have to tell you, labor was such a positive experience for me. I cannot say that it was "painful." It was incredibly hard work. It was exhausting. It felt like my body was working harder than it ever had with every contraction. But I never felt the need for medication or "pain relief." After all, I'd come in at 6 centimeters, I had progressed to about 8, and very soon — I thought — I'd be getting ready to push and meet Daniel. I felt so good, and so empowered about everything.
During the late stages, the part they call "transition," between 8 and 10 centimeters, I entered a sort of trancelike world. I remember that I was kneeling on some soft towels at the side of the bed, leaning over onto my favorite pillow from home, rocking my hips back and forth during every contraction and and breathing through the intensity, barely aware of my surroundings. It was pretty surreal ... they say endorphins kick in at a certain point, and I think they were in high gear then. Nature's narcotics.
Unknown to me, our doula took a picture. It's pretty wild to see what I looked like then:

Then things started to go wrong. First, I stalled out at 8 centimeters, and for several hours, my cervix refused to open any more. Then my cervix started to get swollen. The nurse (the negative one) got the doctor, and at around 2 a.m., they came in and told us what was going on. For some reason, my contractions weren't doing the job well enough, and my cervix was not cooperating. Daniel's head was already sliding into place, and they suspected it might have been turned in a cock-eyed direction. They could already tell he was facing sideways or backwards, so delivery was going to be difficult as it was, unless the boy turned on his own at the last minute. (My friend Kerry tells me this is what happened with her son Quinn, and the fact that he turned was what spared her a Cesarean section.)
For the first time, someone mentioned that I could be headed for a c-section, and I was like, "Huh?" The doctor said the only option he could see that might help prevent one was to put me on pitocin — a drug that mimics the body's natural oxytocin and strengthens and intensifies contractions. I was so low on energy at this point that I knew I wouldn't be able to handle pitocin without an epidural, which the doctor also recommended. The doctor left us for a few minutes to discuss amongst ourselves. I felt out of my depth by now. I had no idea what to make of my swollen cervix or my baby's cocked head. The situation felt alarming, and we didn't know if it would get worse and cause more damage. We decided to go ahead with the pitocin and epidural.
So at about 3 a.m., the anesthesiologist came into the room and administered the epidural. Oops — did I say epidural? I mean, the full spinal block! Yes, he made a mistake and hit the wrong part of my spine, and I soon was so numb that the nurses had to move me around like a rag doll. So I lay there for an hour and a half waiting for the spinal block dose to wear off, and finally he gave me the epidural, correctly this time. It didn't hurt too badly, but needles and anything related to the spine have always freaked me out, so it was ... kinda scary. But the epidural did feel good once it kicked in, I have to say that. It felt good to finally rest.
For another 12 hours, I labored like that — comfortable with the contractions but hooked up to tubes, forced to lie on my right side or left side, hoping and hoping that my cervix would spread open and let Daniel through.
First, it didn't look good: I regressed to 7 inches of dilation. But then the swelling went away, and I dilated back up to 8, even to 9, or even 10 in some parts of the cervix. But not all of the cervix. Hour after hour, the doctor checked me, and no matter how much parts of it dilated fully, there remained a stubborn lip that refused to push back. And therein lie the problem: The doctor did not want to try to push Daniel's head through a cervix that wasn't completely dilated, for fear of worse damage.
Meanwhile, even through the epidural, I was feeling the urge to push. God, how I wanted to push. But I just let the feeling hang in the air and didn't do anything.
We were coming to a turning point. By 2 p.m., I hadn't had anything to eat since the previous afternoon, and I was being hydrated only by an IV line. Daniel was doing just fine, though — his heartbeat never faltered the entire time. Finally, the doctor said, "Let's give it one more hour and see if that lip goes away." I asked if I couldn't just keep on laboring indefinitely, but he told me the pitocin was really giving my uterus a workout, and it wasn't going to be able to go on forever. He told me that was how "women on the prairies" lost their babies or died during childbirth themselves. I wasn't sure whether to believe him, but I didn't have enough information to know for sure. Our doula didn't have any experience with this kind of situation, either. At a certain point, we were going to have to make the call as to whether to have a c-section. The hour passed. The lip did not go away. Frustrated and exhausted, and not sure if continuing to labor would accomplish anything, I agreed to a c-section.
The nurse turned off the pitocin and the epidural drip. Soon, I started to feel my natural contractions again, and this time, they made me angry. I cussed and swore at them. Why should I have to go through these when they're all for nothing, when they aren't going to bring me my baby, I asked Stephen and our doula, finally near tears.
They said our doula could come be with me in the operating room with Stephen. He kissed me goodbye, and I was brought in to prep alone. That part was the hardest. I was scared of what to expect, and even though I felt as if we'd exhausted all our options and made as informed a decision as we could, I was still bummed that all my hard work — and months of preparation and hopes and visions of a natural, drug-free birth — was resulting in the one outcome I'd most hoped to avoid. A c-section seemed so cold and clinical and sterile and ... scary.
But in the end, it wasn't scary. It was so happy. When Stephen and our doula joined me at last, the doula reminded me that I was still having a baby, that a birth was about to happen. That helped me feel less scared. Even better, my regular OB happened to be starting his on-call shift the hospital, so he came to assist at the surgery. It was nice to hear his familiar, grandfatherly voice. And when I felt the procedure start, the reality of it hit me, and I started to cry as I clutched Stephen's hand — tears of joy, not fear: "We're about to meet our baby!" We stared into each other's eyes until suddenly I heard a huge, lusty cry, and there he was — our big boy, born 5:01 p.m., weighing 8 pounds and 9.75 ounces, 21 inches long. (He was born with a sloped head, due to his position in my pelvis, but it went away in a day or two.) Stephen stood up to see over the blue surgical screen. He looked like a big, angry, coneheaded baby, Steve said later. They brought him behind the screen to show us before cleaning off the blood, and it was just amazing and miraculous. I was sobbing. And when our OB proceeded to sing "Happy Birthday" to Daniel, and the rest of the staff joined in, even our doula was teary-eyed.
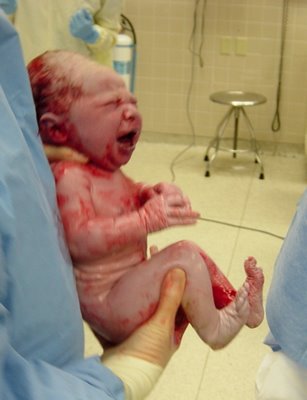
After they cleaned Daniel, they let Stephen and I spend some time holding him behind the screen, and that was when I first got to touch him and kiss him and cry over him. I think my husband had some tears of joy, too. (I cried with pride, too, when they told us his two APGAR scores — which test the baby's functions at birth and five minutes of age — were 9 out of 10. And no one gets 10s. That's my overachiever!) Stephen and Daniel left together, with the doula and cameras in tow, to go to the nursery and get him weighed and tested.

Meanwhile, I was wheeled to recovery — which happens to be right next door to the tub room where I'd labored the night before. Within two hours, Daniel was back in my arms, and I started to nurse him. That was another amazing moment. If I ever had any doubts about my ability to breastfeed, they went away when Daniel went rooting around for his dinner and found it. He is the most eager and lusty little breastfeeder I could have imagined! Thank God my milk supply is meeting his demand. Although he lost a little weight before my milk came in, he had gained back his birth weight and more as of yesterday. Way to go, Daniel!

So that's it. Daniel is hungry now, so I must go. :)






8 comments:
Wow, what an amazing journey. And the great thing is that the rest of the journey is just beginning. I'm so proud of you! You endured amazing things and produced a perfect little boy (even if he was a conehead!) Even if things didn't go as planned the ending is still a beautiful one!
Emilie & Steve -- Congratulations on the birth of Daniel Joseph! He is so cute and looks very healthy.
Emilie, I am amazed that you remember everything during labor & delivery with such clear detail... that is amazing to me.
That is great news that he is breastfeeding so well and I hope that you love it as much as I did, Emilie.
Best wishes,
Megan, Gordon & Katie
It was great to read Daniel's birth story! It actually sounds kind of similar to my experience with Isaac. I was dialated to 10, but his head was cock-eyed as well. I had difficulty withe epidural/spinal as well and then endedup having a c-section. I'm SOOO glad your little boy is here and is doing well. Congrats on the nursing... Daniel is super cute. :)
Wow wow wow. Emilie, you were so strong and brave, and I admire you SO much for all you did to get Daniel out into our world. I am so proud of you. I am sitting here in tears reading your story. It is amazing and so wonderful. So much love and joy. *sniff*. Daniel is GORGEOUS, just perfect, and I am so thrilled for your new family! Happy Birthday, Daniel!!!!!!!!
Thanks for posting that - you really did seem to get to try a little of everything with your labor! I'm glad you had such a postivie natural experience and then also that your c-section went so well. Reading your story eased my fears of a medicated birth a little.
I'm glad that Daniel is a strong nurser! Enjoy these first few weeks with him!
First off, congratulations on your new son! We haven't met, but I'm good friends with your sister, Susanne and she forwarded the link to your blog as we have had similar birth stories with our first born children, sons, and c-sections. I'm very impressed with your blog site and enjoyed reading the volumous journaling you have managed to put forth--as I'm also a new mom, and I know showers are rare and wonderful events these days, let alone time needed to document the precious moment your life changed! Your candid sharing of your experience was comforting to me since you and I shared many of the same troubles. Our son, Andres-Jose, was born on July 6, and we are overjoyed with the task at hand in becoming tempered in the arts of parenting. Please feel free to check out our story by visiting our website at:
www.babyavillanueva.com
In closing, congratulations again on your new beautiful son--life amazes, doesn't it? You seem to be very loving parents who deserve this blessed gift. And thank you for allowing others to connect and feel comforted by the truths that link us together.
The "big, angry conehead" is here! I am so proud of you for getting through this, and for Steve for being there each moment. It's touching that so many other women have gone through similar experiences. My friend Vanessa gave brith 3 weeks ago to a boy (Nigel), after a 30-some-hour labor! His head was also turned the wrong way and stuck in the cervix so he came out coneheaded too. She almost had a cesarian but at the last minute, while she was alone with the doc and her husband, she felt one more try coming on and it finally came through.
You are lucky that he took to breastfeeding right away.
Thank you for the pictures.
When can we meet him?
What an incredible story. Thank you for sharing it! I am really so inspired by your attitude throughout the whole thing. You are a strong and amazing woman! I'm so happy that you felt cared for at United, and your doula sounds wonderful. And such a happy ending! :)
Post a Comment